STARR Study Group, Meuffels, D. E., &...
New publication
STARR Study Group, Meuffels, D. E., &...
New publication
Arens T, Melick van N, van der Steen MC, Janssen...
Editor’s Pick Prof Stafano Zaffagnini Journal of Experimental Orthopaedics
Osteotomy
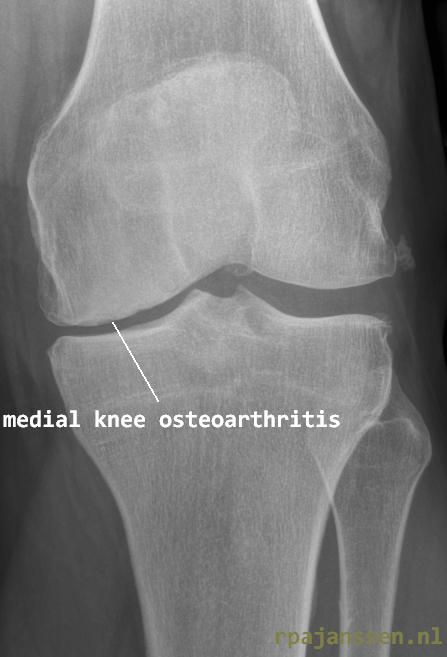
Osteotomy is an operation to correct a bone axis. It may be performed in various bones of the skeleton. Osteotomies are most often performed in the proximal tibia in knee disorders. The main indications are medial knee osteoarthritis and chronic posterolateral knee instability. On this webpage, I will explain leg alignment, the relationship with osteoarthritis and knee instability, surgical procedure, rehabilitation, complications and patient contact information after the surgery.
Human legs may have a straight, varus (O shape) or valgus (X shape) alignment. Leg alignment is genetically determined and may vary with age and activities. Scientific evidence suggests that varus alignment increases in childhood soccer players.
Varus leg alignment may lead to osteoarthritis of the medial side of the knee. The cartilage becomes thinner and pain occurs in loading activities such as sports, walking and running. Bicycling generally leads to less pain than running. In these patients, the medial meniscus has often been removed in previous surgery due to knee injuries. An osteotomy may be a good treatment for medial knee pain in younger pateints (<60 years with an active lifestyle). Osteotomies were less popular in the last century due to necessity of casting for long periods of time. There was a lack of solid material to fix the osteotomy correctly. Nowadays, solid plates (with angular stable screws) are available that allow immediate knee motion with progressive weightbearing after the surgery. Cast is no longer necessary. This new surgical technique has led to excellent results after tibia osteotomy in medial knee osteoarthritis.
Posterolateral knee instability
Ligaments provide stability of the knee. These ligaments are the anterior and posterior cruciate ligaments and both medial and posterolateral ligament complexes. Scientific evidence suggests that medial and posterior cruciate ligaments may heal well if recognised early and adequately treated by an orthopaedic surgeon (see Information Cruciate ligament and Cases Acute posterior cruciate ligament injury). The anterior cruciate ligament and posterolateral complex have a low healing potential. Posterolateral instability is a severe knee injury. This injury often has associated posterior ligament injury but may also be seen in combination with anterior cruciate injuries. Main symptoms are giving way sensations. Sports are difficult to perform. Correct diagnosis of these combined ligamentous injuries are essential for adequate treatment and longterm prognosis. Leg alignment is important in patients with chronic posterolateral instability of the knee. Varus alignment leads to progressibe lateral thrust of the knee with gait disturbances. Solitary reconstructions of the cruciate ligaments rapidly fail if the posterolateral instability is not treated. The best primary treatment option for patients with chronic posterolateral instability with varus alignment, is an osteotomy of the tibia. My practice is a tertiary referral center for these knee pathologies in the South of the Netherlands (see Biography).
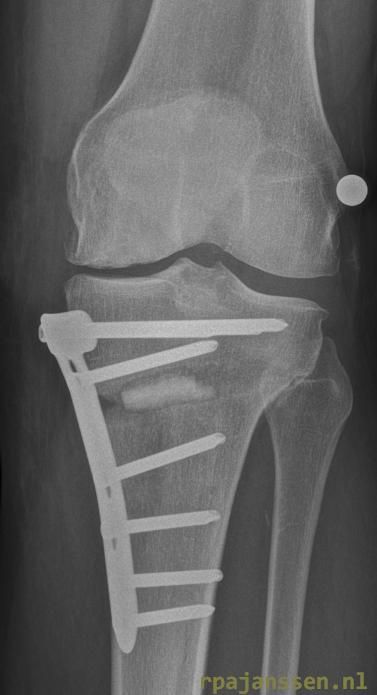
The surgical technique is identical in treatment of both medial osteoarthritis and posterolataral instability. Prior to the operation, the correction is calculated on long weightbearing X-rays. A incision is made in the proximal lower leg. A saw cut is made partially through the tibia and an opening wedge alignment correction performed. A titanium plate and angular stable screws are mounted. During surgery, the amount of correction as well as plate positioning are checked by X-ray. After the surgery, a drainage tube and bandage is put in place.
You are allowed to move your knee freely in flexion and extension after the surgery. Bandage and drain are removed on the first day after the operation.The physiotherapist teaches you to walk with two crutches with partial weightbearing. Leg extension exercises are important to restore normal gait pattern. This will take some practice in the first few weeks. Hospital stay is 3 days. After hospital discharge, you may continue the exercise program with a local physiotherapist. It is recommended to elevate the leg a few times a day for the first few weeks to limit lower leg swelling. Antithrombotic prophylaxis is given for the first 6 weeks. Full weightbearing is allowed after 6 weeks. Hometrainer exercises are allowed if the knee bends sufficiently to cycle. This is a good modality to practice knee flexion. Bone healing in the opened wedge may take up to one year. The first outpatient check-up will be at 2-4 weeks. X-ray examinations will be performed at various times of outpatient appointments.
Comlications after osteotomy are rare (1%). These may be: woundhealing problems, infection, thrombosis. compartmentsyndrome or vascular/nerve injuries. Bone healing is difficult if patients smoke. It is important to stop smoking prior to an ostetomy to minimize the chances of pseudoarthrosis.
Please contact our office in case of:
-
leakage from the wound
-
redness or increase of lower leg pain
-
fever (> 38.5º Celcius).